00389 2 3091 484
00389 2 3091 484
Publication of Petar Ugurov, MD: ”Early initiation of hemofiltration – extracorporeal blood purification in Covid-19 patients″
October 8, 2020
On 22.09.2020, Zan Mitrev Clinic received a new publication on topic “Early Initiation of Extracorporeal Blood Purification Using the AN69ST (oXiris®) Hemofilter as a Treatment Modality for COVID-19 Patients: a Single-Centre Case Series.
This is our original work and the first publication in the Republic of North Macedonia when it comes to COVID – 19, and it was published in the prestigious Brazilian journal of cardiovascular surgery.
The team that worked on this publication is composed of experienced specialist doctors (cardiologists, anesthesiologists, microbiologists, transfusiologists) from the Zan Mitrev Clinic, led by Petar Ugurov, MD.
Petar Ugurov, MD answered several questions related to this research conducted in our clinic and the importance of its application, especially when it comes to patients’ safety, health and fast and safe recovery.
What was the main reason for starting research in this field and what makes this study so specific and significant?
Petar Ugurov, MD – The main reason for our research work is the SARS-CoV 2 virus itself, a virus that has become a challenge for the whole world.
We already know that COVID-19 is a disease caused by SARS-CoV-2, a virus of the Coronavirus family, which was first discovered in China in December 2019.
Before talking about this study, I would like to explain once again how the virus itself leads to deterioration of the general health condition in patients with SARS – CoV2 virus.
The respiratory dysfunction in COVID-19 patients is associated with changes in the respiration mechanics. Decreased mobility of the diaphragm and chest, decreased contraction of the respiratory muscles, and decreased motor activity of the patient may occur. This leads to impaired pulmonary ventilation and gas exchange.
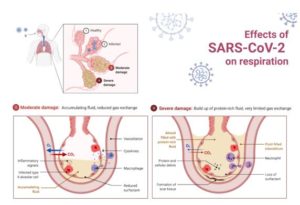
When COVID-19 patients start coughing and have a fever, it is a sign that the infection has reached the respiratory system.
The protective layer of these respiratory organs is damaged, leading to inflammation, and even the slightest amount of dust can cause coughing.
– What makes this study unique and important is that we are the only clinic in the country and a rare one in the region that managed to show how to prevent the progressive deterioration of the general health condition with early initiation of extracorporeal blood purification in combination with systemic heparinization and respiratory support through a specially designed treatment protocol for SARS CoV2 patients.
How did you come up with the idea to start this study?
Petar Ugurov, MD – The study we started to work on and the very idea of this study is based on our previous experiences and work with patients with elevated inflammatory markers, as well as patients in septic shock.
The main challenge that we posed to ourselves is how to prevent the progressive deterioration of the general health condition of SARS – CoV-2 patients.
- We based the overall treatment of COVID-19 patients on the fact that if we have control over the inflammatory markers, then we could have control of the general patient condition, as well as the cytokine storm.
Can you tell us more about the study?
Petar Ugurov, MD – Our study included a group of 15 patients positive for SARS – CoV-2 virus. The continuous monitoring of the level of inflammatory markers, cytokines, and differential blood counts along with D-dimers, LDH, and ferritin, is a powerful predictor of when to initiate haemofiltration as part of the treatment in Covid-19 patients.
Treatment consisted of early initiation of extracorporeal blood purification using the AN69ST (oXiris®) Hemofilter, systemic heparinization, and respiratory therapy.
During this period, we became quite interesting to the general population with the haemofiltration we use and I would like to briefly explain how to use these filters and their function.
The filter we use is oXiris®, which uses a modified AN69ST membrane and which has an affinity for both endotoxins and cytokines. This filter has a three times bigger adsorption power for endotoxins and cytokines.
Additionally, the oXiris set is authorized by the US Food and Drug Administration to treat patients with Sars – CoV2 virus.
- If we go back to our beginnings and to what I mentioned earlier, i.e., how we came up with the idea to start treating patients this way, we will understand that this is actually the way we established control over the inflammatory markers of the cytokine storm.
There has been a lot of talk about the cytokine storm during this period. Can you explain to us what a cytokine storm is and what worries us most about this condition?
Petar Ugurov, MD – Cytokine storm syndrome refers to over-release of cytokines in response to external stimuli and is a major cause of acute respiratory distress syndrome as well as multiorgan failure.
When there is an increased cytokine level, such as of TNF-α, IL-6, IL-1 and IFN, it can cause pathological reactions such as diffuse damage to the alveoli, formation of the so-called transparent membrane and pulmonary fibrosis.
Circulating cytokines can cause widespread endothelial dysfunction with disseminated intravascular coagulation (DIC) and multiorgan failure.
What might be the conclusion of this study and why is it so specific and important?
Petar Ugurov, MD – From the study itself, it can be concluded that early initiation of blood purification using an oXiris® haemofilter may be an effective way to prevent abnormal levels of inflammatory markers in COVID-19 patients.
Also, the continuous monitoring of the vital parameters, biochemical, immune markers as well as coagulation factors and X-rays gives us the opportunity to monitor the severity of the disease and allows us to adjust therapy.
The combination of systemic heparin and extracorporeal blood purification using cytokine-absorbing haemofilters can reduce hyperinflammation, prevent coagulopathy, and support clinical recovery.